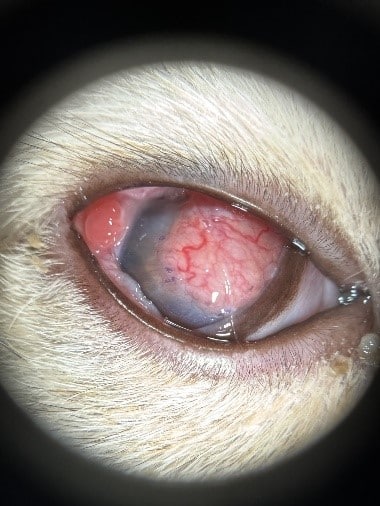
HISTORY: Oats, is a 4-month-old, intact male, Scottish Straight, who presented to Westford Ophthalmology department with concerns for a possible corneal perforation in the right eye. His littermate has mild symptoms of ocular tearing and occasional sneezing. The owner had been treating a corneal ulceration OD and noted bloody ocular discharge, a visible corneal protrusion and moderate pain. He has been rubbing his right eye. Oats was seen initially at urgent care for ocular discharge OU and treated with topical antibiotic and oral clavamox. 11 days prior to referral, Oats was rechecked by his primary care veterinarian. Examination revealed severe conjunctival inflammation, and a dorso-lateral corneal ulceration. An injection of convenia and meloxicam was administered sub-Q in hospital, and he was sent home with ofloxacin ophthalmic suspension (OD TID) and oral meloxicam.
OPHTHALMIC EXAMINATION: Oats retained light perception OD, with a positive dazzle reflex, and negative menace, and was visual OS. Schirmer tear test-1 values were not evaluated OD due to visible corneal perforation and were 11mm wetting/min OS. Intraocular pressure was estimated via a rebound pro-tonometer to reveal a low value of 2.2mmHg OD and normal value of 9.6mmHg OS. Fluorescein stain was positive for a large corneal perforation OD, which was not actively leaking at this time (seidel negative), and was negative OS. Jones test (evaluating patency of the nasolacrimal duct) was negative OU, as no fluorescein stain was appreciated in the nose or mouth.
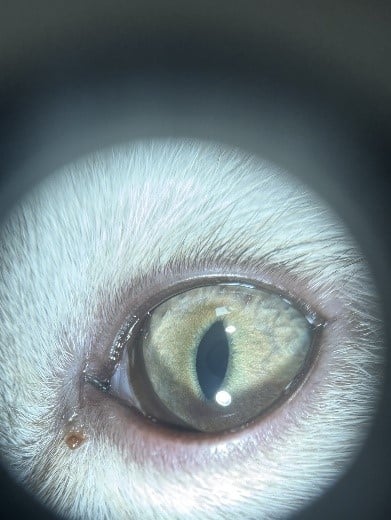
OS: The left eye was open and free of hyperemia. There was mild, nasal pigmented discharge and the left eye otherwise examined normally.
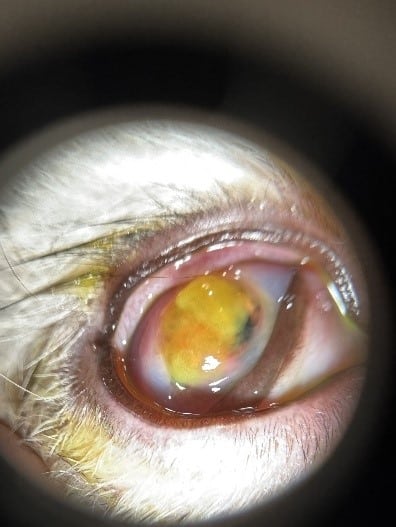
Diagnostics:
Corneal cytology OD was obtained after application of topical proparacaine with a cytobrush. The sample was rolled onto a glass slide and stained with Diff-Quick for in-hospital evaluation. This revealed corenal epithelial cells, 2+ cocci bacteria and 3+ neutrophils.
Aerobic corneal culture OD was submitted to IDEXX laboratory. This revealed no growth.
Oats was diagnosed with a complex, septic, malacic corneal perforation (seidel negative) with uveal prolapse. Treatment options were discussed with the owner to include:
1) Surgical conjunctival pedical grafting OD. This procedure has upwards of a 95% success rate at saving the eye.
Complications were discussed to include Infection, graft dehiscence, uveitis, along with risks of general anesthesia.
2) Aggressive medical therapy. A success rate of 30-50% was discussed. Kittens do have a remarkable healing ability, if the infection is controlled.
After discussion the owner opted for aggressive medical therapy, with a plan to move forward with surgery if there is no improvement, or if the eye re-ruptures.
We discussed that given the history; ocular symptoms and the complex corneal ulceration are likely due to feline-herpes virus-1, with secondary bacterial infection resulting in a complex corneal ulceration.
Conjunctivitis in the cat is most often infectious in nature, where feline herpes virus-1 (FHV-1) infection is thought to be the most common cause. That said, calici virus, mycoplasma and chlamydophila are other known pathogens known to result in conjunctivitis. Other causes of conjunctivitis do exist and include dry eye and allergic conjunctivitis to name a couple.
FHV-1 is a viral infection which is almost endemic in cats as 95% of cats have been exposed. This virus is feline specific and is not contagious to people or other species of animals. The virus is passed to the affected cat at birth or from a cat who has the virus through sneezing, coughing, grooming etc. as is spread by bodily fluids such as saliva or urine. Once the cat has herpes, 80% of cats become latent carriers. The virus can become inactive (latent) and hide in the nerves of the face and at times may re-activate to cause clinical symptoms which can range from conjunctivitis, corneal ulceration and upper respiratory symptoms. 50% of cats whom are latent carriers can have disease flare ups life-long.
Chronic infection of feline herpes virus-1 causes inflammation of the cornea (keratitis), dry eye and symblepharon. Symblepharon is an adhesion of the conjunctiva to itself or to the cornea. Other conditions which may be associated with FHV-1 are corneal sequestrum (dead area of corneal tissue) and eosinophilic keratitis (an immune-mediated condition affecting the cornea).
Definitive diagnosis of FHV-1 is accomplished by laboratory testing. This testing is problematic as there can be false negative results and cats which may be in the carrier state, although not showing clinical signs, may test positive.
Treatment for FHV-1 includes topical or oral anti-viral therapy along with topical antibiotics to treat secondary bacterial infection and topical lubrication as cats can develop a qualitative tear film abnormality (dry eye) for up to 30 days post infection. Topical antiviral medications need to be given frequently, as they slow the virus down, but do not kill the virus. The goal of treatment is to control clinical signs and improve comfort and it is important to note that there is no cure for FHV-1. Once a cat shows signs of infection, they will remain infected for life. Some cats will never show clinical disease after initial infection, while others harbor the virus in a carrier state with recurrent infections. Some cats require symptomatic therapy for recurrent infections, while others show transient clinical signs which only last a few days and do not require therapy. Oral L-lysine is an amino acid dietary supplement which may be effective at controlling re-activation of the virus as has been shown to inhibit viral replication in a laboratory setting. Although studies are lacking in proving its efficacy many believe this amino acid may reduce FHV-1 outbreak frequency and severity. There are no known side effects in giving oral L-Lysine 500mg dose twice daily with food for adult cats.
TREATMENT: *E-collar to prevent rubbing/self-trauma*
Moxifloxacin Oph Solution 0.5% OD Q2 hours ; Cefazolin compounded in artificial tears OD QID; Ophthalmic Serum OD Q2 hours (give last); I-drop OS BID; Famciclovir 62.5mg PO BID X 14 days; AmoxiClav 31.25mg PO BID X 7 days; Gabapentin 10mg PO q8-12 hours X 14 days; Metacam PO q2 4 hours; Proviable probiotic
RECHECK (2 days later): The owner reported that the eye was still squinting, although discharge is now clear and no longer mucoid.
Oats retained light perception only OD and was visual OS. IOP was estimated via a rebound pro tonometer to reveal values of 0.0mmHg, 21.0mmHg in OD and OS respectively. Fluorescein stain was positive for a large, corneal perforation OD-actively leaking today (seidel positive) and negative OS. Jones test was positive OU.
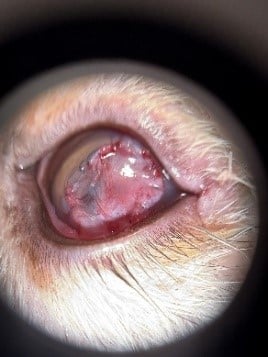
OD: Moderate blepharospasm, palpebral and bulbar conjunctival hyperemia with chemosis and clear periocular discharge. The third eyelid was moderately elevated and hyperemic. There was a large, corneal perforation with uveal prolapse and vascular tissue plugging the defect. The perforation was leaking today. There was mucoid, sticky discharge covering the defect. There was moderate pan stromal corneal edema. Intraocular examination was not possible.
OS: The left eye was unchanged.
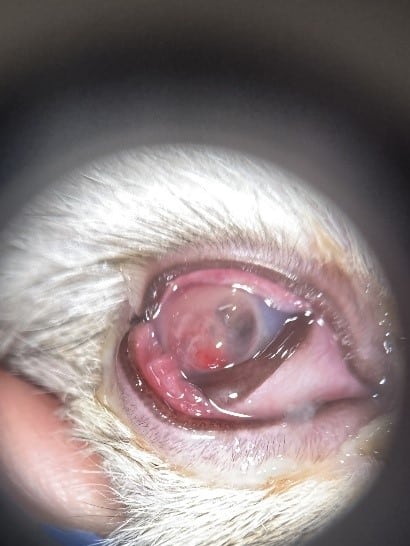


CONJUNCTIVAL PEDICAL GRAFT SURGERY: The surgery was performed under the operating microscope and general anesthesia, with our board-certified anesthesiologist. IV Paralytic (rocuronium) is given to keep the globe central for surgery and requires the patients to be maintained on a ventilator for respiratory support. The infected corneal tissue was debrided, and a conjunctival graft was harvested from the dorso-temporal conjunctiva, keeping a pedicle attached to maintain blood supply. The uveal tissue was replaced intraocularly, and iris adhesions were broken down when possible. As this was a full-thickness corneal perforation, a synthetic Biosis disk was cut to size and sutured over the rupture. The graft is sutured in place with very small, 9-0 vicryl suture.

Dr. Penelope Buechner our board-certified ophthalmologist

Dr. Amanda Crawford our board-certified anesthesiologist